Unwinding of PHE for Medicaid in Missouri: August Update
When the Public Health Emergency (PHE) ended, states began the process of "unwinding" those who gained Medicaid coverage during the PHE. Here is a preliminary analysis of the unwinding data in MO.
UPDATE FOR AUGUST 2023.
The process of recertifying enrollment in Medicaid, which generally had been done on an annual basis before the COVID pandemic, was paused during the Public Health Emergency (PHE) by federal law in early 2020. This meant that those enrolled in Medicaid during that period were not disenrolled. Federal law passed at the end of 2022 called for an end to the PHE, and a renewal of the recertification process, commonly called the “unwinding” of the pandemic as it is affecting Medicaid.
Nationwide Medicaid enrollment rose to a record high during the pandemic, and in Missouri the enrollment also rose to over 1.5 million, a record.
The first three months of data have now been reported by the state of Missouri in a public dashboard. The state also reported by law to the Centers for Medicare and Medicaid Services (CMS). The numbers for Missouri can be compared to other states using, for example, the Kaiser Family Foundation’s unwinding website, which is being continuously updated. This post will review some of the major conclusions from this data, largely drawn from the table attached, computed by this author from the state’s dashboard.
Some major points:
In August, almost 114,000 Medicaid recipients were reviewed (see table). Over the first three month (June-August 2023) about 336,600 of the Medicaid recipients have been reviewed. The state’s plan is to review the total set of enrollees over a 12-month period.
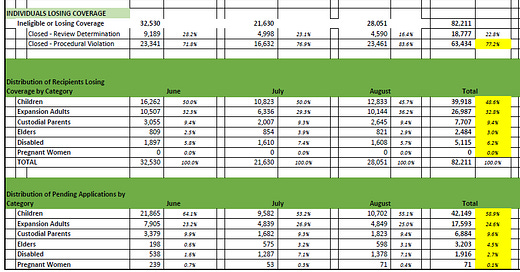
In August, 58.3% of recipients have been determined still eligible for Medicaid, while 28,051 (24.6%) have been declared ineligible or lost coverage. Another 19,421 are pending review. Over the first three months 82,211 (24%) have lost coverage and 54% have remained eligible, while 71,563 cases are still pending.
Of those losing coverage in August, 83.6% lost coverage for a “procedural violation” according to the state, which can be due to a range of reasons, while 16.4% lost coverage because they were no longer eligible for the program. Over the first three months, 77.2% lost coverage for procedural reasons as opposed to being declared ineligible for coverage. The “procedural reasons” is a metric being used widely to measure how states are doing (see Kaiser’s analysis).
Of the total persons losing coverage in August, 46% (12,833) were children, 36% (10,144) were expansion adults, with the rest in other categories (see table). Over the first three months, almost half of those losing coverage have been children (39,918, 49%), 32% are from the adult expansion group (26,097), 9% are custodial parents (7,707), 6.2% are disabled (5,115), and 3% are aged/elders (2,484).
In August, almost 70% of those declared eligible to remain on Medicaid were approved by “ex parte” (the state’s records demonstrated that they were still eligible), and 30% were declared eligible by application to the state. Over the first three months, comparable numbers are 77% and 23%.
In August, 55% of the pending applications were children and 25% were expansion adults. Over the first three months, 59% of the pending applications (42,149) were for children, 25% were from expansion adults (17,593), with the rest in other categories. Reports from the state suggest that the pending application numbers will be updated at a later time.
Source: author’s analysis of unwinding data from https://dss.mo.gov/mis/clcounter/